I’ve stopped life-saving medication says man exhausted by fight for NHS care

Social Affairs Producer
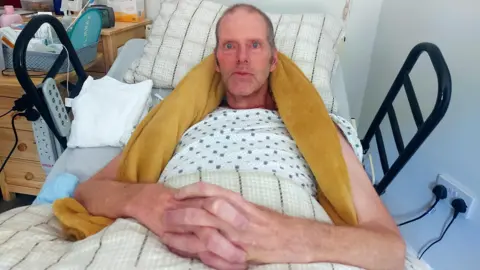 BBC
BBCTim Hull may indicate many successes for 56 years. He directed his own repairman and hosted Ukrainian refugees for two years. Even in the Guinness Book of Records: He and his brother, about 7FT height, have been the longest twins in England for almost twenty years.
But a life that Tim decides to end. He says the quality of life is “very, very low”. Tim, a medical condition that weakens his muscles – unrelated to his height – and his health has decreased rapidly in the last two years.
Tim, wars to get health and care support that pushes him to make a desperate decision, Tim says. He feels that he was abandoned by health professionals, moved from one waiting list to another, the right equipment was not provided to help him, and he has been connected to the bed for about seven months.
In February, he stopped taking the drug that prevented his kidneys from failure. Now they’re starting to give up and he knows it’s for months to live, even if not weeks.
“I don’t think things will be better than that,” BBC News says. “I just feel [ending my life] It would be a better option than lying in bed for 24 hours a day. “
The neurological state of TIM is rare, but most of the challenges are familiar to many people.
For the last two years, BBC News has been contacted by families with more than 250 serious disabled or illnesses about the struggle for access to health and care services.
Many explained the effect of very long wait for evaluations, appointments and vital equipment that can help them cope at home.
They also emphasized the frustration of emphasizing someone’s signing the right services, switching from department to department and the feeling they rested when they reached only one crisis.
For some, there were long arguments as to whether their maintenance would be paid by NHS or local councils.
Tim, who lived on his own on his own, first went to the GP in 2022 because he started to stumble as he walked.
It was directed to a rheumatologist. He waited for a year to say that his appointment was only wrong expertise.
He then waited a few months to see a local neurologist, then waited a few more months to see a senior neurologist in Birmingham. In these two years, he lost his walking ability and had to use a wheelchair.
In the end, TIM was diagnosed with a rare neurological condition, hereditary spastic paraplegia (HSP), causing spasms and muscle weakness. Pain, fatigue and depression are also common symptoms.
It cannot be cured, but according to the NHS website, it usually does not affect life expectancy. There are more than 80 variants, but Tim says it is not yet said to have. Physiotherapy and drugs are often used to manage symptoms, but after the team was diagnosed, he felt that he was expected to “continue with him” only after being diagnosed.
He spent two months in the hospital in 2024. While there, regular physios helped gain some mobility, but there was no ongoing support after being discharged. The case was directed to Worcester and Neurology Therapy team.
TIM received a letter dated 10 July 2024 and that welcomes it and said it was on the waiting list for an assessment. He says he hasn’t heard of anything, even though he makes an appointment. A year later, he received almost the same letter on July 15, 2025. Welcome, you are on a waiting list. This time it contained a information brochure.
 Given
GivenWhen Tim asked for help, he said that his case was often said to be many experts and should call 111.
Tim’s height contributed to the difficulties. For someone with 6FT 10 (2.08m), it seemed impossible to make the foundations correctly.
He used all his savings to adapt his home and buy equipment to live the lower floor, but spent two years in a standard hospital bed provided by NHS, who was very small for him. He describes this as “disgusting disturbing” and “torture”. Three months ago, a new, longer bed was given, but it causes him to sit in a position where he says he said it caused a great drowning time. Now they mostly have food drinks.
It was also a big problem finding a crane to take him inside and out of the bed. The first two tried by NHS were too small to be used safely.
At the end of April, there was a discussion about putting a ceiling crane. They are still waiting. This means that TIM has not been able to leave his bed since February this year.
In addition, it is waiting to hang out for a wheelchair that can cope with her neck, but it cannot be until it becomes a crane to lift it out of bed.
“Life lies only in a bed, feels very uncomfortable, fights to get support,” Tim says. “Over a certain height, you don’t exist.
Im I was living as I was. I couldn’t see myself better and I decided that I didn’t want to be here anymore, or he says. Health and care system, “It didn’t work. There is no combined thought. Nobody cares.”
Authorities responsible for TIM, they say that they cannot comment on individual cases, but regularly review how each individual is looked at to meet their “unique needs”.
Herefordshire and Worcestershire Health and Care NHS Trust, “Equipment, home compliance or community nursing support is necessary, we aim to make them in place [before discharge] To provide a safe, well -supported transition from the hospital to home “.

Tim has a separate, hereditary kidney condition called polycystic kidney disease. Twin Andy was born with his fathers who took their fathers and nun sue.
Twenty years ago, Tim had a kidney transplant from his brother Richard. TIM should stop the kidney failure twice a day.
Without them, the team knows that he has been left to live for months, even if not weeks. He thinks he has other options than to stop buying tablets.
Sue, a retired child’s social worker, says that he is ruined by TIM’s decision.
“He doesn’t have to die here. There is much more to give, or he says. “And I just feel completely abandoned.”
Almost every day he spends looking at him and made endless calls to try to get the support he needed.
In February, Sue made urgent calls because TIM’s GP’s GP was very low for local mental health services and adult social services. Again, he said he was sent from the column and that it was a fight to get help. “No combined thought,” he says.
Tim says he doesn’t regret six months after stopping the tablets.
But he put pressure on what makes a difference, “If I were to be thrown out [of bed] And he sat for dinner, if I can just go to the garden to get a landscape change, it can help. “
A friend of mine suggested that Sue had to contact the local nursing home. Now it has become the central advice, support and information that TIM desperately needed two years ago. He manages Ağrı drugs and helped him get NHS financing for four maintenance visits per day. He also organized to check that a psychologist has the capacity to make an end -of -life decision.
He says that he asked this question several times by clinicians, but no one asked what could be done to rethink him.
He doesn’t get lost in the tragic irony Sue, in which he goes to end -of -life care to get more combined help, but he says it’s still not enough to provide the level of support it really needs.
Orum I definitely feel broken from the situation, or he says. “I think I went beyond anger. I can’t believe that Britain will allow it to happen.
 Given
Given“We are working in close partnership with other health and care organizations to ensure a combined care experience of patients. Multi -disciplined teams (MDTs) bring professionals from different experts to regularly review the needs of each patient,” TIM’s local NHS Trust says.
NHS Herefordshire and Worcestershire Integrated Maintenance Board (ICB) says that “make sure that it meets the needs of patients and is both safe and effective”. He also says that “responding to any concern, learning from events and continuous improvement in the whole system” is net systems.
ICB says “everyone is seen, heard and supported, regardless of their individual conditions,” he says.
The Ministry of Health and Social Care (DHSC) says that “Mr. Hull is unacceptable that he doesn’t get the care he deserves” and he’s working to ensure that everyone can reach high quality care.
DHSC, 10 -year health plan “patients and their families to get personalized care in the right place to ensure that the health services will shift to the community of the society,” he said. He also says that he has invested 100 million pounds for the hospital and the end -of -life care.
Tim is now very weak and very strong painkillers. When he leaves, he adds “he wants to be as comfortable and supported as possible” and “there is more fear than the unknown” with the decisions I make “.
If you are experiencing distress or despair, help and support details in the UK BBC Action line.





